what is Staphylococcus aureus:-
Staphylococcus aureus, a type of bacteria often found in various illnesses, can cause different sicknesses in people. These infections happen often, whether someone gets sick outside or inside the hospital. It’s tricky to treat them because some bacteria don’t respond to many medicines, such as MRSA ((Methicillin-Resistant Staphylococcus aureus).
Normally, this bacteria doesn’t make healthy skin sick. But if it gets inside the body or the bloodstream, it can cause some pretty serious infections. This article talks about (what is Staphylococcus aureus) and how doctors check and treat these infections. It also talks about how important it is for a team of different healthcare professionals to work together when someone has these sicknesses.
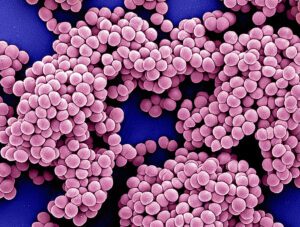
Body parts are affected by this infection:-
Various types of staph bacteria can create problems in different areas of your body. Staphylococcal infection might affect:
- Skin: The most common staph bacteria, Staphylococcus aureus, can lead to skin issues like boils, blisters, and redness. These skin problems can pop up anywhere, especially around the mouth and nose.
- Breasts/Chest: People who breastfeed might encounter mastitis, causing swelling and pus-filled pockets in their breasts.
- Digestive System: Consuming contaminated food could trigger food poisoning, resulting in vomiting and diarrhea.
- Bones: Staph bacteria can cause bone inflammation and pain, a condition known as osteomyelitis.
- Lungs and Heart: Infections in the lungs, such as pneumonia and breathing difficulties, can occur if these bacteria invade. They can also harm heart valves, potentially leading to heart failure.
- Bloodstream: When staph bacteria release toxins into your body, it can cause severe infections like septicemia, also known as blood poisoning
Risk Factor:-
Several factors can increase the likelihood of staphylococcal infections:
- Influenza
- Chronic lung conditions like cystic fibrosis or emphysema
- Leukemia
- Presence of tumors
- Having undergone a transplant or using implanted medical devices such as artificial heart valves, joints, or heart pacemakers, or having a catheter for a long time
- Burns
- Open wounds or sores
- Persistent skin conditions
- Recent surgery
- Diabetes mellitus
- Chronic kidney disorders needing dialysis
- Use of medications like corticosteroids, immunosuppressants, or cancer chemotherapy
- Radiation therapy
- Illicit drug injection
- Newborns and breastfeeding mothers
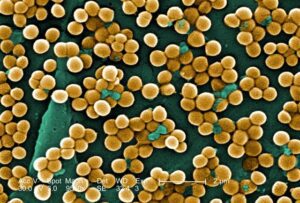
staphylococcus aureus symptoms:-
When Staphylococcus aureus affects the skin, it can result in various conditions:
- Folliculitis: This is the mildest form, causing a small, slightly painful pimple at the base of a hair where the follicle gets infected.
- Impetigo: It leads to shallow blisters filled with fluid that break and leave honey-colored crusts. Impetigo may cause itching or discomfort.
- Abscesses (Boils or Furuncles): These are painful, pus-filled lumps under the skin’s surface.
- Cellulitis: This infection spreads, causing pain and redness in the skin and underlying tissue.
- Toxic Epidermal Necrolysis and Scalded Skin Syndrome: These severe infections lead to extensive peeling of the skin. Toxic epidermal necrolysis affects adults, while scalded skin syndrome occurs in newborns
Staphylococcal skin infections spread easily.
After giving birth, mastitis (breast infections) can emerge within 1 to 4 weeks, causing redness and pain around the nipple. Abscesses might release bacteria into the mother’s milk, potentially affecting the nursing infant.
Pneumonia brings a high fever, breathing troubles, and a cough with blood-tinged sputum. Lung abscesses may form, making breathing even harder.
In severe burns, bloodstream infections are a common cause of death, showing as persistent high fever and sometimes shock.
Endocarditis damages heart valves rapidly, leading to heart failure and severe breathing issues.
Osteomyelitis causes chills, fever, and bone pain, with redness and swelling in the surrounding skin and tissues, possibly affecting nearby joints.
Diagnosis:-
How a staph infection is found depends on where it’s located in your body. While visible on the skin, doctors use special tests like Gram stain and bacterial cultures to confirm it. Here’s how they identify it:
- Skin: Doctors look at the affected area and might take a skin sample for testing.
- Food poisoning: They ask about your symptoms and how long you’ve been sick, sometimes needing a stool sample.
- Mastitis: Doctors check for symptoms and might test your milk for bacteria.
- Toxic shock syndrome: They take urine or blood samples and might do a CT scan to check your organs.
- Endocarditis: Doctors consider symptoms, do blood tests, and might do an echocardiogram.
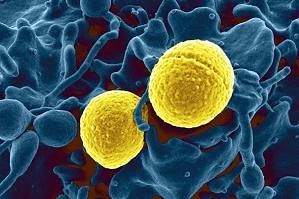
staphylococcus aureus treatment:-
Treatment for Staphylococcus aureus infections often involves antibiotics and, in some cases, surgery to remove infected bone or foreign materials. Here’s how doctors treat these infections:
- Hospital-Acquired Infections: Treated with antibiotics effective against MRSA, like vancomycin, linezolid, and others. If susceptible to methicillin and no penicillin allergy, drugs like nafcillin or oxacillin might be used. Treatment duration varies based on infection severity, sometimes lasting weeks.
- Community-Acquired MRSA: Usually responsive to different antibiotics like trimethoprim/sulfamethoxazole, clindamycin, or doxycycline, similar to hospital-acquired MRSA treatment.
- Mild Skin Infections: Folliculitis and similar issues are often treated with over-the-counter ointments or prescription-based mupirocin. More severe cases may require oral or intravenous MRSA-effective antibiotics.
- Bone or Foreign Material Infections: Rifampin might be combined with other antibiotics. Surgical removal of infected material, like pacemakers or artificial joints, is typically needed for a complete cure.
- Abscesses: When present, doctors usually drain abscesses as part of the treatment.

Prevention:-
Hand Hygiene:
A simple yet highly effective measure is thorough handwashing with soap and water. Alternatively, using alcohol-based hand sanitizers can help eliminate staph bacteria, especially after contact with potentially contaminated surfaces.
2. Nasal Treatment Caution:
While some doctors prescribe the antibiotic mupirocin to clear staphylococci from nasal passages, its overuse can lead to resistance. Hence, this treatment is typically reserved for situations with a higher infection risk, such as before specific surgeries or in households where skin infections are spreading.
3. Precautions Before Surgery:
Individuals identified as carriers of staphylococci often receive antibiotics before undergoing certain surgeries. This preemptive measure aims to minimize the risk of infections linked to these bacteria.
4. Managing Infections:
Anyone with a staphylococcal skin infection should refrain from handling food to prevent the potential spread of bacteria.
5. Healthcare Facility Measures:
Some healthcare facilities adopt screening practices upon admission to detect MRSA (Methicillin-Resistant Staphylococcus aureus) among high-risk individuals, especially those gearing up for specific procedures. The screening involves a simple nasal swab. If MRSA is detected, isolation measures are promptly initiated to prevent further transmission.
By adopting these straightforward practices, individuals can play a significant role in reducing the spread of staphylococci bacteria. These steps not only safeguard personal health but also contribute to a healthier environment for everyone
Also learn about What Is Autism Spectrum Disorder? 4 Types of Autism Spectrum Disorder-Symptoms, Causes & Treatments
